Search News
TerraVista Metrics (TVM)Industry Portal
TerraVista Metrics (TVM)Hot Articles
TerraVista Metrics (TVM)- RCEP Glamping Tents Carbon Mutual Recognition Extended to PhilippinesRCEP Glamping Tents carbon mutual recognition now extends to the Philippines — faster customs, 67% lower testing costs, and green procurement advantages. Act now!
- EN 16798-2:2026 Enforcement Starts May 1, 2026EN 16798-2:2026 enforcement starts May 1, 2026—key for AI HVAC, occupancy sensors & smart curtains in EU hotels. Act now to avoid market access risks!
- ADQ Launches $180M Phase II for China Supply Chain Localization in UAEADQ launches $180M Phase II fund to localize China’s glamping tent, modular cabin & RV component supply chain in UAE — apply by June 1, 2026.
Popular Tags
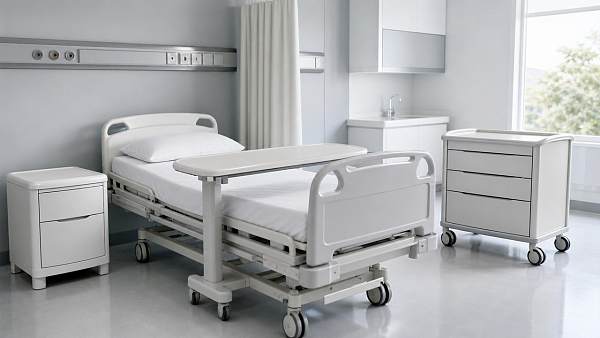
TerraVista Metrics (TVM)Industry NewsHospital Furniture Choices That Affect Cleaning Efficiency
auth.Dr. Hideo Tanaka (Outdoor Gear Engineering Lead)Time
May 07, 2026Click Count
In healthcare environments, hospital furniture plays a bigger role in cleaning efficiency than many teams realize. For quality control and safety managers, the right choices can reduce contamination risks, simplify maintenance workflows, and support compliance with strict hygiene standards. From surface materials to structural design, every detail affects how fast and how thoroughly spaces can be cleaned.
Why cleaning efficiency starts with hospital furniture
Cleaning efficiency in hospitals is often discussed in terms of chemicals, staffing, training, and disinfection protocols. Those elements matter, but they do not work in isolation. Hospital furniture directly shapes how easily environmental services teams can access surfaces, remove soil, prevent moisture retention, and verify that cleaning has been completed to standard. A poorly designed bedside table, chair, storage cart, or treatment couch can add friction to every cleaning cycle.
For quality control and safety managers, this issue is operational rather than cosmetic. Furniture decisions influence turnover time, cross-contamination risk, audit performance, and long-term maintenance costs. In high-demand healthcare settings, small inefficiencies multiply quickly. If surfaces include deep seams, exposed fasteners, porous laminates, or low-clearance bases, staff spend more time cleaning and may still struggle to achieve full coverage.
That is why hospital furniture should be evaluated as part of the infection prevention system. It is not simply interior equipment. It is a daily-contact infrastructure layer that affects hygiene reliability, safety outcomes, and cleaning labor efficiency.
What hospital furniture means in a hygiene-focused context
In a healthcare setting, hospital furniture includes patient beds, bedside cabinets, overbed tables, waiting chairs, nurse station seating, medication carts, trolleys, examination couches, wardrobes, worktops, and storage units. When viewed through a cleaning-efficiency lens, the most important question is not appearance or even initial comfort. It is whether the item supports fast, repeatable, verifiable cleaning under real operating conditions.
The strongest designs usually share several traits: smooth non-porous surfaces, minimal horizontal dust traps, sealed joints, corrosion-resistant frames, rounded edges, and accessible undersides. These features reduce residue buildup and lower the chance that pathogens remain hidden in hard-to-reach zones. Good hospital furniture also withstands repeated exposure to detergents and disinfectants without blistering, cracking, fading, or releasing particles.
This is where a metrics-based approach becomes useful. Organizations such as TerraVista Metrics emphasize the value of raw technical data over visual claims. In healthcare-adjacent procurement logic, the same principle applies: furniture should be assessed by cleanability, material endurance, and compatibility with rigorous sanitation cycles, not by brochure language alone.
Why the industry pays closer attention today
Several healthcare trends have increased scrutiny on hospital furniture. First, infection prevention standards are more visible and more heavily documented than before. Second, hospitals face pressure to improve room turnover without compromising safety. Third, modern facilities are integrating smart equipment, modular room layouts, and sustainability targets, which means furniture must perform well across hygiene, durability, and lifecycle criteria at the same time.
There is also a growing recognition that hidden maintenance burdens undermine operational performance. Furniture that looks suitable on installation day may degrade quickly under disinfectant exposure, frequent movement, and intensive use. Once finishes chip or seals fail, cleaning becomes less effective and replacement costs rise. For safety managers, that creates a compliance issue. For quality teams, it creates variability that is difficult to control.
In other words, hospital furniture is now part of a broader risk-management discussion. It sits at the intersection of infection control, workplace efficiency, patient safety, and asset stewardship.
Core design factors that affect cleaning performance
Not every furniture specification has equal impact. Some details consistently determine whether cleaning teams can work efficiently and whether surfaces remain hygienic over time.
Surface material and finish
Non-porous, chemical-resistant surfaces are easier to clean and less likely to harbor moisture or stains. Smooth healthcare-grade polymers, sealed compact surfaces, coated metals, and high-quality stainless steel often perform better than absorbent or textured materials. Finishes should resist common disinfectants, including alcohol-based and chlorine-based products where applicable.
Joint construction and seam control
Open seams, exposed screw heads, and layered edges create micro-traps for dust, fluids, and biological residue. Sealed joints and simplified construction reduce cleaning complexity and improve visual inspection. This matters especially in high-contact furniture near patients.
Geometry and access
Rounded corners are not only safer; they are also easier to wipe thoroughly. Elevated designs with adequate floor clearance support mop access and reduce manual repositioning. If cleaning tools cannot easily reach the underside or rear frame, contamination risk increases.
Mobility and stability
Furniture on casters can improve access, but only if wheels are easy to clean and do not accumulate debris. Locking mechanisms should be robust and simple. Unstable items create safety concerns and discourage frequent movement, which then limits proper floor and wall-edge cleaning.
Durability under sanitation cycles
The best hospital furniture remains intact after repeated cleaning. Material fatigue, delamination, corrosion, and cushion cracking all reduce hygiene performance. Quality teams should treat durability data as a cleaning variable, not just an engineering one.
A practical overview of furniture features and cleaning impact
Furniture feature Cleaning impact Risk if poorly specified Seamless top surfaces Faster wipe-down and easier disinfection coverage Fluid ingress, residue retention, staining Rounded edges and corners Reduces missed spots and supports safer handling Dirt accumulation in sharp joins, impact damage Chemical-resistant finish Maintains surface integrity through repeated cleaning Peeling, cracking, discoloration, rough surfaces Raised base or open underside Improves access for mops and inspection Hidden dust, difficult floor sanitation Easy-clean casters Supports movement and full-area cleaning Debris buildup, poor mobility, inconsistent cleaning Where hospital furniture has the biggest hygiene impact
Not all hospital zones have the same exposure level or cleaning intensity. Quality control teams should prioritize furniture review based on clinical risk, frequency of touch, and cleaning turnover demands.
Patient rooms
Beds, bedside cabinets, overbed tables, visitor chairs, and privacy-related components are touched frequently and cleaned often. Furniture here should support quick disinfection between users and withstand continuous handling.
Emergency and treatment areas
Fast turnover makes cleanability critical. Trolleys, stools, exam couches, and mobile carts should have minimal crevices and high chemical resistance because staff cannot afford long cleaning delays during peak demand.
Waiting and public zones
Although these areas may seem lower risk, they experience high traffic and varied user behavior. Upholstery selection, armrest design, and frame accessibility strongly influence cleaning consistency.
Staff workspaces and support rooms
Nurse stations, storage cabinets, and work chairs still matter. Dust accumulation and poor wipeability can compromise broader hygiene efforts and slow routine maintenance.
How quality and safety managers can evaluate options
A useful evaluation framework should combine observable design review with technical verification. Start by asking whether the hospital furniture can be cleaned thoroughly without disassembly, awkward lifting, or special tools. Then assess whether the materials are validated for your cleaning agents and usage intensity.
Request evidence where possible: chemical resistance data, finish durability results, load performance, caster test results, and maintenance guidance. Products that claim hygiene benefits should be able to show measurable support for those claims. This aligns with a broader infrastructure benchmarking mindset: operational confidence comes from tested performance, not assumptions.
It is also wise to involve environmental services staff in trials. They often identify practical issues that spec sheets miss, such as inaccessible underside bars, wheel housings that trap hair, or handles that slow wipe-down. Their input helps ensure hospital furniture supports real workflows rather than idealized ones.
Common specification priorities by furniture type
Furniture type Priority cleaning criteria Operational note Bedside cabinet Sealed edges, smooth handles, easy-clean wheels High-touch and frequently moved Overbed table Non-porous top, resistant column finish, stable base Food and clinical contact increase contamination risk Waiting chair Wipeable upholstery, open frame geometry High user turnover demands quick cleaning Treatment trolley Minimal seams, chemical resistance, caster hygiene Supports fast-paced clinical workflows Storage unit Dust-resistant top profile, easy-wipe doors, durable hinges Often overlooked but important for routine sanitation Frequent mistakes that reduce cleaning efficiency
One common mistake is prioritizing aesthetics over cleanability. Decorative contours, textured surfaces, and complex frames may suit hospitality spaces, but in healthcare they often slow cleaning and increase risk. Another mistake is assuming all antimicrobial or healthcare-labeled finishes perform equally well. Without durability and maintenance data, those labels may not reflect long-term hygiene performance.
A third issue is separating procurement from environmental services and safety oversight. Hospital furniture should not be selected solely by budget or appearance. It should be reviewed as an asset that affects labor efficiency, contamination control, and lifecycle compliance. Finally, organizations sometimes underestimate replacement timing. Once surfaces are damaged, cleaning efficiency declines even if the furniture remains structurally usable.
Turning furniture choices into a measurable hygiene strategy
The most effective organizations treat hospital furniture as part of a measurable hygiene system. That means setting clear criteria before purchase, testing representative samples in actual cleaning conditions, documenting approved chemical compatibility, and tracking failure patterns over time. If certain caster designs jam, if seat materials crack early, or if seam lines repeatedly retain debris, those findings should feed back into future specifications.
For quality control and safety managers, this creates a stronger basis for decision-making. Instead of reacting to complaints or isolated failures, teams can build a performance database that links furniture design to cleaning time, maintenance frequency, and hygiene audit outcomes. That approach supports better standardization across wards and facilities.
Conclusion and next-step guidance
Hospital furniture affects cleaning efficiency in ways that are easy to overlook but difficult to correct later. The right choices improve access, reduce contamination traps, withstand harsh sanitation routines, and make cleaning results more consistent. For healthcare quality and safety leaders, that makes furniture specification a practical risk-control decision, not a secondary design matter.
If your facility is reviewing hospital furniture, begin with the items that combine high touch frequency, demanding cleaning cycles, and visible maintenance issues. Use measurable criteria, involve frontline cleaning staff, and favor tested performance over surface-level marketing. In environments where hygiene standards must be proven every day, better hospital furniture is not just easier to clean. It helps make the whole care environment more reliable.
Recommended News
![Orthopedic Implants Selection Often Hinge on Long-Term Fit Orthopedic Implants Selection Often Hinge on Long-Term Fit]() May 07, 2026Orthopedic Implants Selection Often Hinge on Long-Term FitOrthopedic implants selection depends on proven long-term fit, fatigue reliability, and clinical evidence. Learn what technical evaluators verify before procurement decisions.
May 07, 2026Orthopedic Implants Selection Often Hinge on Long-Term FitOrthopedic implants selection depends on proven long-term fit, fatigue reliability, and clinical evidence. Learn what technical evaluators verify before procurement decisions.![]() May 07, 2026Pharmacy Equipment Upgrades That Reduce Dispensing ErrorsPharmacy equipment upgrades can sharply reduce dispensing errors, improve traceability, and strengthen compliance. Explore the best systems for safer, more reliable pharmacy operations.
May 07, 2026Pharmacy Equipment Upgrades That Reduce Dispensing ErrorsPharmacy equipment upgrades can sharply reduce dispensing errors, improve traceability, and strengthen compliance. Explore the best systems for safer, more reliable pharmacy operations.![Nebulizers for Daily Use: What Actually Matters Most Nebulizers for Daily Use: What Actually Matters Most]() May 07, 2026Nebulizers for Daily Use: What Actually Matters MostNebulizers for daily use: discover what really matters most—consistent medication delivery, easy cleaning, quiet operation, and reliable comfort that fits your routine.
May 07, 2026Nebulizers for Daily Use: What Actually Matters MostNebulizers for daily use: discover what really matters most—consistent medication delivery, easy cleaning, quiet operation, and reliable comfort that fits your routine.![Hospital Furniture Choices That Affect Cleaning Efficiency Hospital Furniture Choices That Affect Cleaning Efficiency]() May 07, 2026Hospital Furniture Choices That Affect Cleaning EfficiencyHospital furniture choices can make or break cleaning efficiency. Discover which designs reduce contamination risk, speed disinfection, and support safer, more compliant healthcare spaces.
May 07, 2026Hospital Furniture Choices That Affect Cleaning EfficiencyHospital furniture choices can make or break cleaning efficiency. Discover which designs reduce contamination risk, speed disinfection, and support safer, more compliant healthcare spaces.![]() May 07, 2026Home Healthcare Setup Mistakes That Create Daily RisksHome healthcare mistakes can create daily risks at home. Discover common hazards, safety fixes, and smart ways to build a safer care setup for loved ones.
May 07, 2026Home Healthcare Setup Mistakes That Create Daily RisksHome healthcare mistakes can create daily risks at home. Discover common hazards, safety fixes, and smart ways to build a safer care setup for loved ones.![DIY supplies shoppers often regret buying too cheap DIY supplies shoppers often regret buying too cheap]() May 06, 2026DIY supplies shoppers often regret buying too cheapDIY supplies can save money—or cost more when cheap tools and materials fail fast. Discover which budget buys shoppers regret most and how to choose smarter for better results.
May 06, 2026DIY supplies shoppers often regret buying too cheapDIY supplies can save money—or cost more when cheap tools and materials fail fast. Discover which budget buys shoppers regret most and how to choose smarter for better results.![Greenhouse supplies that solve heat stress before summer peaks Greenhouse supplies that solve heat stress before summer peaks]() May 06, 2026Greenhouse supplies that solve heat stress before summer peaksGreenhouse supplies that prevent heat stress before summer peaks: explore shading, ventilation, sensors, and cooling solutions for steadier crops and smarter site performance.
May 06, 2026Greenhouse supplies that solve heat stress before summer peaksGreenhouse supplies that prevent heat stress before summer peaks: explore shading, ventilation, sensors, and cooling solutions for steadier crops and smarter site performance.![Flooring materials that look durable but fail in wet areas Flooring materials that look durable but fail in wet areas]() May 06, 2026Flooring materials that look durable but fail in wet areasFlooring materials may look durable, yet many fail fast in wet areas. Learn which options create slip, swelling, and maintenance risks—and how to choose smarter for long-term performance.
May 06, 2026Flooring materials that look durable but fail in wet areasFlooring materials may look durable, yet many fail fast in wet areas. Learn which options create slip, swelling, and maintenance risks—and how to choose smarter for long-term performance.![What slows yield in solar cell manufacturing lines? What slows yield in solar cell manufacturing lines?]() May 06, 2026What slows yield in solar cell manufacturing lines?Solar cell manufacturing yield slows when materials, process control, and equipment stability drift. Discover key risks, QC warning signs, and practical ways to improve consistency.
May 06, 2026What slows yield in solar cell manufacturing lines?Solar cell manufacturing yield slows when materials, process control, and equipment stability drift. Discover key risks, QC warning signs, and practical ways to improve consistency.![Biomass energy projects often stall at this early planning step Biomass energy projects often stall at this early planning step]() May 05, 2026Biomass energy projects often stall at this early planning stepBiomass energy projects often stall before design due to weak fuel, site, and compliance data. Learn a practical framework to cut risk, speed decisions, and improve project delivery.
May 05, 2026Biomass energy projects often stall at this early planning stepBiomass energy projects often stall before design due to weak fuel, site, and compliance data. Learn a practical framework to cut risk, speed decisions, and improve project delivery.![Hydroelectric components that drive most unplanned downtime Hydroelectric components that drive most unplanned downtime]() May 05, 2026Hydroelectric components that drive most unplanned downtimeHydroelectric components that cause most unplanned downtime: learn which parts fail most, how to spot warning signs early, and where to invest for lower outage risk.
May 05, 2026Hydroelectric components that drive most unplanned downtimeHydroelectric components that cause most unplanned downtime: learn which parts fail most, how to spot warning signs early, and where to invest for lower outage risk.![Photovoltaic panels lose output for reasons many sites overlook Photovoltaic panels lose output for reasons many sites overlook]() May 05, 2026Photovoltaic panels lose output for reasons many sites overlookPhotovoltaic panels can lose output from heat stress, connector faults, shading, and mismatch. Learn the overlooked causes and smarter maintenance steps to improve performance.
May 05, 2026Photovoltaic panels lose output for reasons many sites overlookPhotovoltaic panels can lose output from heat stress, connector faults, shading, and mismatch. Learn the overlooked causes and smarter maintenance steps to improve performance.![Eco-friendly gadgets that actually cut energy use at home Eco-friendly gadgets that actually cut energy use at home]() May 05, 2026Eco-friendly gadgets that actually cut energy use at homeEco-friendly gadgets that truly lower home energy use: compare smart plugs, LED lighting, thermostats, and sensors to cut bills, improve comfort, and choose devices with real savings potential.
May 05, 2026Eco-friendly gadgets that actually cut energy use at homeEco-friendly gadgets that truly lower home energy use: compare smart plugs, LED lighting, thermostats, and sensors to cut bills, improve comfort, and choose devices with real savings potential.![AR Glasses Still Have One Barrier to Everyday Use AR Glasses Still Have One Barrier to Everyday Use]() May 04, 2026AR Glasses Still Have One Barrier to Everyday UseAR glasses still face one key barrier to everyday business use: all-day comfort. Explore where they deliver real ROI in hospitality, tourism, training, and operations.
May 04, 2026AR Glasses Still Have One Barrier to Everyday UseAR glasses still face one key barrier to everyday business use: all-day comfort. Explore where they deliver real ROI in hospitality, tourism, training, and operations.![Industrial & Manufacturing Tech Choices That Raise Hidden Costs Industrial & Manufacturing Tech Choices That Raise Hidden Costs]() May 04, 2026Industrial & Manufacturing Tech Choices That Raise Hidden CostsIndustrial & Manufacturing procurement mistakes often hide in durability, integration, and compliance gaps. Learn how to spot hidden costs early and make smarter, lower-risk buying decisions.
May 04, 2026Industrial & Manufacturing Tech Choices That Raise Hidden CostsIndustrial & Manufacturing procurement mistakes often hide in durability, integration, and compliance gaps. Learn how to spot hidden costs early and make smarter, lower-risk buying decisions.![Home Theater Systems Often Sound Bad for One Simple Reason Home Theater Systems Often Sound Bad for One Simple Reason]() May 04, 2026Home Theater Systems Often Sound Bad for One Simple ReasonHome theater systems often sound bad because of poor speaker placement and room acoustics. Learn the simple fixes that boost clarity, bass, and immersion before buying new gear.
May 04, 2026Home Theater Systems Often Sound Bad for One Simple ReasonHome theater systems often sound bad because of poor speaker placement and room acoustics. Learn the simple fixes that boost clarity, bass, and immersion before buying new gear.![Are VR Headsets Finally Comfortable Enough for Longer Sessions? Are VR Headsets Finally Comfortable Enough for Longer Sessions?]() May 04, 2026Are VR Headsets Finally Comfortable Enough for Longer Sessions?VR headsets are becoming more viable for longer sessions—but comfort depends on fit, heat, optics, and use case. Explore what buyers should test before choosing.
May 04, 2026Are VR Headsets Finally Comfortable Enough for Longer Sessions?VR headsets are becoming more viable for longer sessions—but comfort depends on fit, heat, optics, and use case. Explore what buyers should test before choosing.![Why Some Digital Cameras Still Beat Phones in Low Light Why Some Digital Cameras Still Beat Phones in Low Light]() May 04, 2026Why Some Digital Cameras Still Beat Phones in Low LightDigital cameras still outperform phones in low light with cleaner detail, better autofocus, and more natural images. See what makes them the smarter choice for travel and indoor shooting.
May 04, 2026Why Some Digital Cameras Still Beat Phones in Low LightDigital cameras still outperform phones in low light with cleaner detail, better autofocus, and more natural images. See what makes them the smarter choice for travel and indoor shooting.![Forging Services or Machining First? The Cost Tradeoff Forging Services or Machining First? The Cost Tradeoff]() May 03, 2026Forging Services or Machining First? The Cost TradeoffForging services or machining first? Explore the true cost tradeoff for metal components, from strength and lifecycle risk to carbon, compliance, and smarter procurement decisions.
May 03, 2026Forging Services or Machining First? The Cost TradeoffForging services or machining first? Explore the true cost tradeoff for metal components, from strength and lifecycle risk to carbon, compliance, and smarter procurement decisions.![Valve Production Delays Often Start Before Machining Valve Production Delays Often Start Before Machining]() May 03, 2026Valve Production Delays Often Start Before MachiningValve production delays often begin before machining. Learn how specs, supplier qualification, materials, and document control impact lead times—and how to reduce costly project risk.
May 03, 2026Valve Production Delays Often Start Before MachiningValve production delays often begin before machining. Learn how specs, supplier qualification, materials, and document control impact lead times—and how to reduce costly project risk.![Wireless Chargers That Look Fast but Charge Inconsistently Wireless Chargers That Look Fast but Charge Inconsistently]() May 03, 2026Wireless Chargers That Look Fast but Charge InconsistentlyWireless chargers may look fast, but many fail in real use. Discover how to spot stable, cooler, more reliable wireless chargers before you buy.
May 03, 2026Wireless Chargers That Look Fast but Charge InconsistentlyWireless chargers may look fast, but many fail in real use. Discover how to spot stable, cooler, more reliable wireless chargers before you buy.![Gear Manufacturing Tolerances That Affect Long-Term Wear Gear Manufacturing Tolerances That Affect Long-Term Wear]() May 03, 2026Gear Manufacturing Tolerances That Affect Long-Term WearGear manufacturing tolerances directly influence wear, noise, and reliability. Learn which precision factors matter most for long-term performance and smarter component decisions.
May 03, 2026Gear Manufacturing Tolerances That Affect Long-Term WearGear manufacturing tolerances directly influence wear, noise, and reliability. Learn which precision factors matter most for long-term performance and smarter component decisions.![When Tooling and Fixtures Start Slowing Production When Tooling and Fixtures Start Slowing Production]() May 03, 2026When Tooling and Fixtures Start Slowing ProductionTooling and fixtures slowing production? Learn how to spot hidden bottlenecks, reduce quality and delivery risks, and make smarter supplier decisions for scalable projects.
May 03, 2026When Tooling and Fixtures Start Slowing ProductionTooling and fixtures slowing production? Learn how to spot hidden bottlenecks, reduce quality and delivery risks, and make smarter supplier decisions for scalable projects.![Smart classroom solutions are easier to buy than to integrate well Smart classroom solutions are easier to buy than to integrate well]() May 02, 2026Smart classroom solutions are easier to buy than to integrate wellSmart classroom solutions are easier to source than to integrate well. Discover how compatibility, scalability, and data-driven evaluation reduce risk and improve deployment success.
May 02, 2026Smart classroom solutions are easier to buy than to integrate wellSmart classroom solutions are easier to source than to integrate well. Discover how compatibility, scalability, and data-driven evaluation reduce risk and improve deployment success.
Quarterly Executive Summaries Delivered Directly.
Join 50,000+ industry leaders who receive our proprietary market analysis and policy outlooks before they hit the public library.